Coagulopathy in Trauma
Contributed by: Prof. Roman Dudaryk, MD; Professor of Clinical Anesthesiology and Trauma Anesthesiologist, University of Miami Miller School of Medicine and Ryder Trauma Center
Introduction: From the Vicious Triad to Endothelial Dysfunction
Coagulopathy is a critical and often early complication of trauma, contributing significantly to hemorrhagic death. Historically, the condition was framed by the “vicious triad” of hypothermia, acidosis, and hemodilution, which were believed to precipitate clotting abnormalities during trauma resuscitation. As a result, clinical strategies emphasized aggressive crystalloid administration with delayed use of blood products, a practice now understood to be detrimental. Recent evidence has shifted this paradigm, revealing that coagulopathy begins at the moment of injury due to endothelial disruption and the activation of endogenous anticoagulant and fibrinolytic pathways [1,2].
Pathophysiology of Trauma-Induced Coagulopathy
Trauma-induced coagulopathy (TIC) is initiated by a cascade of events triggered by tissue injury, hypoperfusion, and systemic inflammatory responses. It is now understood to be a distinct, multifactorial entity with both endogenous and exogenous contributors.
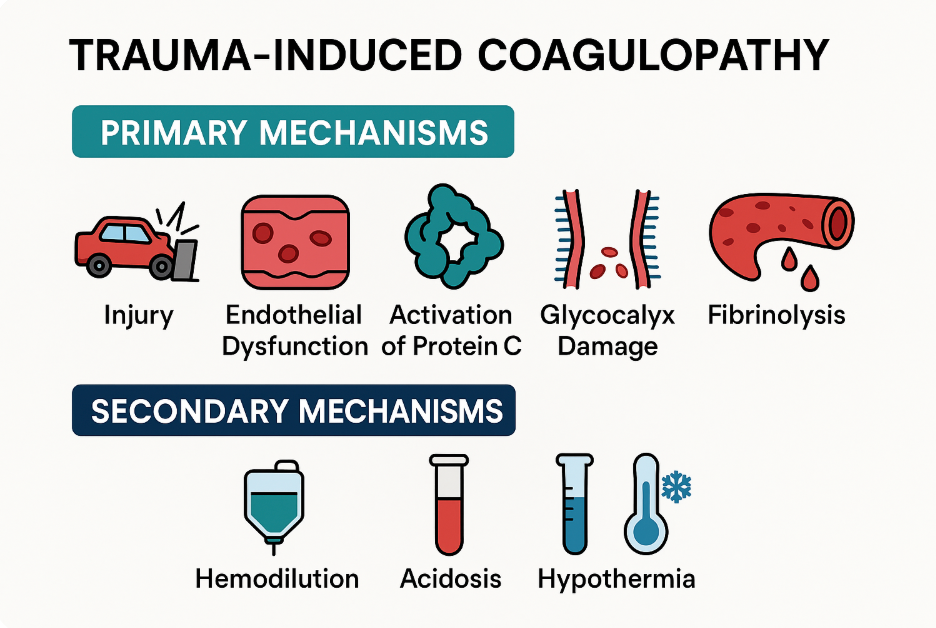
Primary Mechanisms: At the core of TIC is endothelial dysfunction. Blunt or penetrating trauma, coupled with hemorrhagic shock, leads to direct endothelial injury and shedding of the glycocalyx, a protective carbohydrate-rich layer that modulates vascular permeability and coagulation. Loss of glycocalyx integrity exposes subendothelial thrombomodulin and triggers activation of the protein C pathway [2,3].
Once activated, protein C becomes activated protein C (aPC), which exerts potent anticoagulant effects by degrading clotting factors Va and VIIIa, thereby impairing thrombin generation. Concurrently, aPC inhibits plasminogen activator inhibitor-1 (PAI-1), resulting in enhanced fibrinolysis through unregulated tissue plasminogen activator (tPA) activity [3,4].
Fibrinogen consumption and impaired platelet function further amplify the coagulopathy. Within minutes of injury, trauma patients may present with reduced fibrinogen levels, even before significant blood loss. Endogenous catecholamine surge, acidosis, and hypothermia further inhibit enzymatic clotting cascades and platelet aggregation [5].
Secondary Mechanisms: Resuscitation-Induced Coagulopathy In addition to endogenous dysregulation, TIC is worsened by resuscitation-induced coagulopathy, including excessive crystalloid use, inadequate warming leading to hypothermia, and dilution of coagulation factors from unbalanced transfusion. Each of these iatrogenic contributors can aggravate existing deficits in coagulation and fibrinolysis, compounding the severity of bleeding [6].
Subphenotypes of TIC: Emerging evidence suggests that TIC is not a uniform process but may manifest as distinct subtypes, including:
- Hyperfibrinolytic (excessive clot breakdown)
- Hypocoagulable (impaired clot formation)
- Mixed phenotype (features of both)
Viscoelastic testing such as thromboelastography (TEG) and rotational thromboelastometry (ROTEM) allows for early identification of these phenotypes, guiding targeted resuscitation strategies [7].
Importantly, patients who survive the initial hypocoagulable phase may transition into a prothrombotic state in the ICU, increasing the risk for deep vein thrombosis, pulmonary embolism, and organ failure due to microvascular thrombosis [8].
Figure 1: Primary and Secondary Trauma-Induced Coagulopathy
Laboratory evidence supports this mechanism, with abnormal prothrombin time (PT) or activated partial thromboplastin time (aPTT) seen in up to 30% of trauma patients on arrival, correlating with a 35% increase in mortality [1].
Evolving Resuscitation Strategies: From Component Therapy to Whole Blood
Observational studies and military experience prompted a shift toward balanced transfusion strategies. A retrospective study of 246 patients in Iraq demonstrated improved outcomes with a 1:1 ratio of plasma to red blood cells (RBCs), supporting early hemostatic resuscitation [9].
The landmark PROPPR trial (Pragmatic, Randomized Optimal Platelet and Plasma Ratios) compared 1:1:1 versus 1:1:2 transfusion ratios. Although no statistically significant difference in 24-hour or 30-day mortality was found, 1:1:1 was associated with reduced death from exsanguination and minimized crystalloid use. Despite being underpowered, its findings shaped current massive transfusion protocols [4].
Building on these lessons, recent practice has increasingly embraced whole blood (WB) for trauma resuscitation. WB simplifies logistics, reduces donor exposure, and provides balanced hemostatic components in a single product. Military and prehospital experience have driven its resurgence, with observational data suggesting improved outcomes [10].
Figure 2: Whole Blood vs Component Therapy

Future Directions and Ongoing Research
Interest in whole blood has sparked a new wave of clinical research aimed at refining its use in both prehospital and hospital settings. The COMBAT trial is evaluating low-titer group O whole blood administered in the field for patients with major hemorrhage. PPOWER is examining whole blood versus standard component therapy in trauma patients transported by air. Meanwhile, the SWAT study is assessing integration of whole blood protocols across regional trauma systems.
In parallel, efforts are underway to refine viscoelastic-guided resuscitation, develop reliable predictive tools for identifying TIC phenotypes, and explore pathogen-reduced whole blood products for expanded civilian use. These research initiatives aim to close current knowledge gaps and standardize best practices for trauma resuscitation across diverse care settings.
References
- Shaz BH, et al. Anesth Analg. 2009;108(6):1760–1768.
- Brohi K, et al. J Trauma. 2003;54(6):1127–30.
- Maegele M, et al. Crit Care. 2017;21(1):84.
- Holcomb JB, et al. JAMA. 2015;313(5):471–82.
- Cotton BA, et al. J Trauma. 2009;66(1):41–49.
- Cap AP, et al. Transfusion. 2015;55(S2):115S–123S.
- Matijevic N, et al. J Trauma Acute Care Surg. 2013;74(1):69–75.
- Chang R, et al. Lancet Haematol. 2016;3(12):e575–82.
- Nessen SC, et al. J Trauma. 2013;75(2 Suppl 2):S197–S203.
- Spinella PC, et al. Transfusion. 2009;49(2):276–281.

